June 12, 2025
When we talk about healthy habits, we often focus on nutrition, mental health, or overall fitness. But what about your feet? These often-overlooked heroes carry you through life — and they deserve some attention, too.
Incorporating a few gentle foot mobility drills into your morning routine can help improve flexibility, reduce stiffness, and set you up for a pain-free day. Let’s explore a few simple daily foot exercises that support longevity and mobility, all in under 10 minutes.
Why Morning Foot Rituals Matter
After a night of rest, it’s normal for your feet to feel stiff or tight. That’s because circulation slows down when we sleep, and our muscles and joints aren’t being used. A quick morning routine for foot health helps:
Improve blood flow
Gently wake up foot muscles
Prevent long-term issues like plantar fasciitis or joint stiffness
Support better balance and stability throughout the day
Plus, it feels great — and your feet will thank you!
Your 5-Minute Morning Routine for Foot Health
These beginner-friendly exercises can be done from your bed, the bathroom counter, or even while you’re waiting for your coffee to brew.
1. Toe Spreads (1 minute)
https://youtube.com/shorts/gOwgyrmU6hM?feature=shared
Sit or stand comfortably. Spread your toes apart as wide as you can, then release. Repeat 10–15 times.Why it helps: Improves foot strength and activates the smaller intrinsic foot muscles that support balance.
2. Ankle Circles (1 minute per foot)
https://youtu.be/qaatVpZy2ek?feature=shared
Lift one foot off the ground and gently rotate your ankle clockwise 10 times, then counter-clockwise 10 times. Switch feet.Why it helps: Promotes circulation and joint mobility to counteract morning stiffness.
3. Towel Curls (1–2 minutes)
https://youtu.be/toqnSys_JRw?feature=shared
Place a small towel on the floor and try to scrunch it toward you using just your toes.Why it helps: Strengthens the arches and enhances coordination in the foot muscles.
4. Calf Stretch with Wall or Step (1–2 minutes)
https://youtu.be/utLavyPDnqI?feature=shared
Stand with your hands on a wall or place your toes on a step while your heel stays on the ground. Lean forward until you feel a stretch in your calf and Achilles tendon. Hold for 20–30 seconds per leg.Why it helps: Loosens up the back of the leg and heel — essential for preventing plantar fasciitis and Achilles tendonitis.
Bonus: Gentle Foot Massage
https://youtu.be/BwhGFoHDkUI?feature=shared
Before putting on your socks or shoes, use your thumbs or a massage ball to roll out the soles of your feet. Focus on tight spots in the arch and heel. Just 1–2 minutes can make a big difference.
Foot Mobility Drills = Long-Term Foot Wellness
Incorporating these foot mobility drills into your morning can support not just your feet, but your entire body. Improved foot function leads to better posture, less knee and hip pain, and more stability with every step you take.
And remember — consistency is key. Like any good habit, the benefits of daily foot exercises build up over time.
Feature Photo by Aljona Ovtšinnikova
May 29, 2025
When you think of dehydration, you probably imagine symptoms like dry mouth, fatigue, or dizziness—but what about your feet? It may surprise you to learn that dehydration can directly contribute to foot pain, cramping, and even swelling. Since your feet are at the farthest point from your heart, they rely heavily on healthy circulation and fluid balance to function properly.
Let’s take a look at how your water intake affects your feet—and why staying hydrated is more important than you might think.
1. Dehydration and Foot Cramps
If you’ve ever woken up in the middle of the night with a painful foot cramp, dehydration might be the culprit. Proper hydration is essential for normal muscle function. Without enough fluids, your muscles—especially in your feet and calves—can tighten up unexpectedly.
Cramps often occur when your body is low on essential electrolytes like potassium, magnesium, and sodium, which are lost through sweat. Since water helps regulate these minerals, not drinking enough can increase your risk of sudden, painful cramps in the feet.
2. Hydration Supports Circulation in the Feet
Good circulation is critical for healthy feet. Water plays a major role in keeping your blood flowing efficiently. When you’re dehydrated, your blood volume decreases, making it harder for your heart to pump blood to the extremities—including your feet.
Poor circulation can lead to sensations of numbness, tingling, or a “pins and needles” feeling in your feet. In more severe cases, chronic dehydration could contribute to long-term circulatory problems that make foot pain worse over time.
3. Water Helps Lubricate Joints and Reduce Pain
Your feet contain more than 30 joints, all of which rely on synovial fluid for smooth, pain-free movement. Dehydration reduces your body’s ability to produce this fluid, leading to stiff, achy joints—especially in people with arthritis or other joint conditions.
Drinking enough water each day can help reduce joint discomfort and improve mobility in your feet and ankles.
4. Is Water Retention the Opposite Problem?
Interestingly, dehydration can also lead to swollen feet—but not for the reason you might think. When your body senses it's not getting enough water, it holds onto the fluids it does have. This can result in swelling (also known as water retention) in the feet, ankles, and lower legs.
Staying properly hydrated signals your body that it can safely release excess fluids, helping to reduce swelling and bloating in the feet.
5. Tips to Keep Your Feet (and the Rest of You) Hydrated
Aim for 8–10 glasses of water per day, and more if you're physically active or it's hot outside.
Avoid too much caffeine or alcohol, as these can dehydrate your body.
Eat water-rich foods like cucumbers, oranges, and watermelon.
Listen to your body—if you're feeling thirsty, you're likely already slightly dehydrated.
When to Seek Help
If you’re experiencing regular foot pain, cramping, or swelling—especially if increasing your water intake doesn’t help—it’s time to speak with a foot care specialist. At Feet First Clinic, our chiropodists can assess the cause of your symptoms and recommend personalized treatment options to get you back on your feet comfortably.
Final Thoughts
Dehydration doesn’t just leave you feeling tired—it can seriously impact your foot health. From muscle cramps to water retention, the way you hydrate has a direct effect on how your feet feel and function.
So next time your feet are aching or swollen, take a moment to consider your water intake. A simple increase in hydration might be the first step toward relief.
May 15, 2025
Gut Inflammation and Foot Pain – What’s the Link?
Foot pain is often blamed on overuse or injury—but new research highlights a less obvious cause: gut health. Specifically, gut inflammation and foot pain are more connected than you might expect. When the gut lining becomes compromised, harmful particles can leak into the bloodstream, triggering systemic inflammation.
This inflammation may impact muscles, joints, and soft tissues—especially in the feet, where stress is frequent.
Systemic Inflammation and Plantar Fasciitis
One of the most common causes of heel pain, plantar fasciitis, is already driven by inflammation. But when systemic inflammation is present due to poor gut health, it can make symptoms worse and recovery slower.
People with inflammatory diseases like rheumatoid arthritis or inflammatory bowel disease often experience foot pain, suggesting a deeper, whole-body link. Reducing systemic inflammation through gut care may provide relief for conditions like plantar fasciitis.
Gut Microbiome and Joint Health in the Feet
The gut microbiome—the complex ecosystem of bacteria in your digestive tract—plays a critical role in regulating inflammation and immune response. When the microbiome is imbalanced (a condition known as dysbiosis), inflammation can increase, affecting joint health across the body, including in the feet and ankles.
Emerging studies show a strong connection between gut microbiome and joint health, indicating that good gut bacteria may help reduce chronic foot pain linked to inflammation.
Nutrient Absorption: A Key to Musculoskeletal Foot Health
Beyond inflammation, poor gut health also affects how your body absorbs nutrients, such as:
Vitamin D
Magnesium
Omega-3 fatty acids
These nutrients are essential for maintaining strong bones, muscles, and connective tissues. A gut that’s not absorbing nutrients efficiently could contribute to foot fatigue, pain, or slow injury recovery.
How to Support Gut Health for Better Foot Health
If you're dealing with persistent foot pain—especially conditions like plantar fasciitis—supporting your gut could be a game changer. Here are some steps to consider:
Adopt an anti-inflammatory diet: Reduce processed foods, sugar, and excess alcohol.
Add probiotics and fiber: These help maintain a balanced gut microbiome.
Stay hydrated and active: Movement supports both gut motility and foot health.
Get tested: A healthcare provider can check for nutrient deficiencies or inflammatory markers.
By improving your gut health, you may also be reducing the underlying inflammation contributing to your foot issues.
When to See a Chiropodist
Foot pain shouldn’t be ignored. If your discomfort persists despite footwear changes or home remedies, a professional assessment is key. At Feet First Clinic, we look at the bigger picture—including possible systemic factors like gut health that may be influencing your pain.
Final Thoughts on Gut Health and Foot Pain
The body is more interconnected than we often realize. Research on gut inflammation and foot pain, systemic inflammation and plantar fasciitis, and the gut microbiome’s role in joint health is still growing—but one thing is clear: taking care of your gut may help your feet feel better too.
Featured Photo by Sora Shimazaki
April 30, 2025
Finding the best neutral running shoes is an important “step” for runners who want a natural, supported stride. Neutral running shoes are designed for those who don't require extra corrective features and benefit most from balanced cushioning and stability. Many people also look for lightweight running shoes that deliver comfort and speed without feeling bulky. In this guide, we’ll help you find the right pair! Many of these shoes, and others, are available at our Toronto foot clinic, Feet First Clinic, and foot specialists like chiropodists and podiatrists often suggest them for people with a normal gait or who supinate.
https://www.youtube.com/shorts/0bVBNNUAUOc
What are Neutral Running Shoes?
To understand what neutral shoes are, it helps to look at different foot types and the way each moves during walking or running. Foot types are typically defined by the height of the arch and associated gait patterns:
Flat feet: Minimal or no visible arch, often leading to overpronation, where the foot rolls excessively inward during movement. Around 40% of runners overpronate, and without the right shoes, overuse injuries like plantar fasciitis can develop. Runners with flat feet should consider stability shoes, sometimes the more restrictive motion control shoe.
High arches: A very pronounced arch, often leading to underpronation (also called supination), where the foot rolls outward.
Normal arch: A moderate, well-formed arch that’s about “halfway full.” It supports a relatively neutral walking or running gait without excessive rolling inward or outward.
Neutral shoes are designed for individuals with a normal arch and a natural gait, meaning their foot doesn't overly roll in (overpronate). Neutral running shoes are also suitable for people with high arches who underpronate. These shoes prioritize cushioning and shock absorption over structural support or corrective features, offering a more flexible and natural ride.
Unlike stability shoes or motion control shoes, which are more rigid, built to control motion and guide the foot into proper alignment, neutral shoes allow the foot to move more freely and comfortably, simply because this is okay for a normal arch and a normal gait doesn’t need guidance. The focus is on lightweight materials, responsive cushioning, and smooth transitions from heel to toe.
Comfortable neutral shoes are ideal for runners or walkers who have an efficient gait cycle and don’t require additional support to prevent injury. They can also be a good option for individuals with high arches, who often benefit from extra cushioning to protect against the increased impact that comes from less natural shock absorption.
How Do Neutral Shoes Prevent Foot Pain?
Neutral shoes help prevent foot pain by offering ample cushioning and promoting the foot’s natural motion without interference. For people with normal arches and a stable gait, or high arches, too much corrective structure can actually cause discomfort or alter natural biomechanics. Neutral shoes support a smooth stride while providing the soft, consistent underfoot feel needed to absorb the repeated impact of walking or running.
One of the key ways neutral shoes protect against foot pain is by reducing the jarring forces that travel up through the feet and legs with every step via shock absorption. High-quality cushioning materials, such as EVA foam or advanced proprietary foams, spread out impact forces and minimize stress on the heels, arches, and forefoot. This protection helps prevent common issues like plantar fasciitis (heel pain), metatarsalgia (pain in the ball of the foot), and even joint discomfort in the knees and hips.
Additionally, neutral shoes are often lighter and more flexible than stability or motion control shoes, which can reduce fatigue over longer distances. With less weight to lift and more natural foot mechanics, you can stay active longer and more comfortably. The result? A smoother, more enjoyable experience every time you move. And your feet aren’t too tired at the end of the day!
Top Neutral Running Shoes in 2025
Where do you start when you want to find the right pair? Luckily, we’re going to talk about some of the best options. Some of these are available at our Toronto foot clinic, Feet First Clinic, and come highly recommended by chiropodists and podiatrists. You can always call or visit us to determine what high quality footwear we have in stock at any given time.
ASICS Gel-Nimbus 27
The ASICS Gel-Nimbus 27 is a premium neutral running shoe designed for comfort and durability. It features a high stack height of 43.5 mm at the heel and 35.5 mm at the forefoot, providing ample cushioning for long-distance runs and everyday walking. The midsole utilizes ASICS' FF Blast Plus Eco foam, offering a soft yet responsive ride. A PureGel insert under the heel enhances shock absorption, which reduces joint strain. The engineered jacquard mesh upper is both breathable and supportive, contributing to the shoe's overall comfort. Despite its cushioning, the Gel-Nimbus 27 maintains a relatively lightweight profile, making it suitable for daily training.
This model is ideal for runners seeking a plush, cushioned experience during long runs or recovery days. But it's not just for runners! It's also ideal for people with foot pain, arthritis, or who want to keep their feet comfy and supported as they go about their daily activities. Its premium cushioning makes it feel like you're walking on a cloud. Whether you're training for a marathon or enjoying a leisurely jog, this shoe offers the support and comfort needed to keep you going. It's also fantastic for non-runners who just want a comfortable walking shoe.
Saucony Triumph 23
The Saucony Triumph 23 is another top-tier neutral running shoe with a stacked heel, known for its plush cushioning and smooth ride. It features PWRRUN+ foam in the midsole, delivering a soft yet responsive feel underfoot. The shoe's geometry promotes a natural stride, and the updated upper provides a secure, comfortable fit. Its durable outsole offers reliable traction, ensuring confidence on various terrains. Overall, the Triumph 23 combines cushioning, support, and durability, making it a versatile choice for runners and non-runners alike. The cushioning also delivers great shock absorption, while the mid-rocker sole reduces strain on the forefoot - great for people with high arches and joint rigidity.
This shoe is particularly well-suited for runners who prioritize comfort and support over speed. The Triumph 23's design caters to those who spend extended periods on their feet, whether during training sessions or daily activities. Its combination of cushioning and stability makes it a reliable choice for a wide range of runners.
Brooks Ghost
For those who don’t want a stacked heel, the Brooks Ghost is renowned for its balanced cushioning and reliable performance. This neutral running shoe offers a 12 mm heel-to-toe drop, catering to runners who prefer a traditional feel. Its DNA LOFT v3 midsole provides a smooth, responsive ride, while the engineered mesh upper ensures breathability and comfort. The durable rubber outsole enhances traction, making it suitable for various surfaces. The Ghost 16's consistent performance and comfort make it a go-to option for daily training and long-distance runs.
Ideal for runners seeking a dependable and straightforward shoe, the Ghost 16 delivers a comfortable experience without unnecessary frills. Its design focuses on providing a smooth transition from heel to toe, accommodating a variety of running styles. Whether you're a seasoned runner or just starting out, the Ghost 16 offers the support and comfort you need. It's also great for people who wear custom orthotics.
March 27, 2025
Tight calves and foot health go hand in hand (or should we say foot in foot?). Our body parts are intricately connected, meaning discomfort in one area can lead to issues elsewhere. Likewise, muscle strain and fatigue in the lower legs can wreak havoc on the feet and other body parts if ignored for too long. Let’s explore the symptoms and causes of tight calves, how tight calves affect the body and feet, and how a chiropodist or podiatrist can help you manage pain.
Tight Calves: What Are They?
"Tight calves" is a general term describing the sensation of stiffness, pain and tension in the muscles at the back of the lower leg, often leading to restricted movement that affects your daily life. This tightness can manifest as muscle pain and stiffness when walking, balance issues, and more. Tight calves and posture even have a connection!
Anatomy of the Calf Muscles
The calf comprises two primary muscles:
Gastrocnemius: The primary or chief muscle in the calf. It’s located on the back of your leg, relatively close to the skin’s surface. This superficial muscle has two heads, medial and lateral. It helps flex the knee and foot, and also plays a crucial role in walking and posture.
Soleus: Located beneath the gastrocnemius, this wide and flat muscle is deeper, and originates from the posterior tibia while connecting to the Achilles tendon above the heel. This group helps stabilize ankle during activities like walking and running.
Understanding the structure and function of these may be helpful in determining the cause of calf muscle tension.
What Causes Calf Pain?
Pain in the lower part of the back of the legs does not always feel the same. It may come on suddenly, or nag at you all day by way of a mild, dull ache. The former is often the result of a sudden injury or sharp movement, whereas the latter can build over time, resulting from lifestyle choices like wearing unsupportive shoes or working out too hard.
Here are some common causes of calf pain:
Muscle Cramps. Sudden, involuntary contractions of the calf muscles, known as cramps, can cause significant tightness and discomfort. These cramps may result from factors such as dehydration, general muscle fatigue, or electrolyte imbalances.
Overuse. Engaging in repetitive activities that involve a lot of running or jumping can overwork the calf muscles and make them feel tight. This is especially common when increasing training intensity or duration without allowing yourself to rest.
Muscle Strain. Overstretching or tearing the calf muscles, often due to sudden movements or excessive force, can result in tightness, pain, and swelling.
Non-supportive and Ill-fitting Footwear. Shoes lacking arch support, shock absorption, or cushioning force the muscles to work harder with every step. Without proper arch support, the foot may put excessive strain on the calf muscles as they attempt to stabilize the lower leg. A lack of shock absorption further increases the impact of the ground on the feet and legs. Similarly, insufficient cushioning fails to distribute pressure evenly, leading to increased stress on the calves, especially during prolonged standing or walking.
Poor Ankle Mobility. Limited flexibility in the ankle joint can place additional strain on the calf muscles, contributing to tightness. Some causes include having a history of ankle injuries or arthritis.
Pre-existing Gait Abnormalities and Foot Type. Overpronation (excessive inward foot rolling — common in flat feet) or underpronation (excessive outward foot rolling — common with high arches), can lead to calf muscle tightness due to altered mechanics and increased strain.
Dehydration and Mineral Deficiencies. Lack of adequate fluids or essential minerals like potassium, magnesium, and calcium can lead to muscle cramps and tightness in the calves.
Inactivity. Prolonged periods of inactivity or sedentary behavior can cause the calf muscles to become tight due to lack of regular movement and stretching.
Venous Insufficiency. Conditions like deep vein thrombosis (DVT) or varicose veins can cause calf tightness, as well as general venous insufficiency.
How Tight Calves Affect the Body and Feet
We can feel the effects of tight calf muscles in more ways than one. Our feet can become weaker, more vulnerable and fatigued, sometimes leading to a foot condition we didn’t have before. Tight calves can also cause experience mysterious back and knee pain. Here are common additional problems can arise from strain in the lower legs.
Joint Pain
Tight calves can have a significant impact on the body's overall alignment, posture and movement, often leading to joint pain in the knees, back, and feet.
When the calf muscles are tight, they restrict proper ankle dorsiflexion (raising the foot upwards towards the shin). When ankle mobility is restricted, the body may lean forward slightly to maintain balance, causing strain on the lower back muscles and leading to chronic discomfort. This abnormality can put excessive strain on other joints, like in the knees. This perfect storm of joint problems and limited movement can contribute to conditions like osteoarthritis over time.
Biomechanical Foot Conditions
The feet often bear the brunt of tight calf muscles, as they have to absorb additional stress during movement. Calf pain can cause a disrupt our running or walking gait as we try to move through the pain. Further, since our calf muscles connect our knees to our ankles, when the calves become tight it puts strain on the ankle. This disrupts our foot mechanics and can cause painful, chronic overuse injuries like plantar fasciitis and Achilles tendonitis. In fact, tight calves is one of the leading contributing factors to Achilles tendonitis and plantar fasciitis.
Increased Risk of Injury
Aching, tense muscles are more susceptible to further strains and tears, in addition to also causing balance problems as you struggle with pain. All of this combined can be a recipe for disaster and lead to a slip or fall (especially in seniors) that may cause even more damage, like a broken bone. Tight calf muscles can also contribute to more mild conditions like shin splints (repetitive stress on the shin bone) and generally hinder athletic performance.
Circulatory Problems
The calf muscles assist in pumping blood back to the heart from the lower extremities. Tightness in these muscles can impede this process, resulting in swelling in the feet and ankles and, in severe cases, contributing to circulatory problems.
How to Treat Tight Calves: Muscle Tightness and Foot Care
https://www.youtube.com/shorts/sNdIAxZNOn8
A foot care professional can help with calf tightness and pain. With their guidance and your determination to improve your foot and leg health, you can live and move comfortably. Let’s explore some options.
Compression Stockings
Wearing medical-grade compression stockings can improve circulation in the lower legs, reducing muscle fatigue and tightness and giving your lower extremities a healthy, comforting and energizing boost.
They work by applying gentle pressure to the legs, which helps prevent blood pooling and promotes better oxygen delivery to the muscles. Compression therapy is especially useful for individuals who spend long hours on their feet, live a sedentary lifestyle, spend prolonged periods sitting while travelling, pregnant women, or those with conditions like varicose veins. A physician can determine the right level of compression based on your specific needs.
Custom Orthotics
Custom orthotics can help address underlying biomechanical issues that contribute to tight calves. A chiropodist can assess foot structure to design orthotics that conform to your feet, and yours alone, providing tailored support and alignment for your unique needs.
By correcting imbalances and reducing strain on the lower leg muscles, orthotics can help alleviate tightness and prevent further discomfort. These devices can be particularly beneficial for individuals with flat feet, high arches, or abnormal gait patterns that place excessive stress on the calves.
Proper Footwear
Shoes with adequate arch support, cushioning, and shock absorption that redistributes pressure away from the heel can help keep your feet comfortable, maintain proper lower limb alignment and reduce strain on the calf muscles. Chiropodists and podiatrists often advise against wearing unsupportive footwear like flip-flops or high heels for prolonged periods, as they can contribute to muscle tightness and discomfort in the calves and feet.
Strengthening Exercises and Stretching Programs
A structured exercise program focusing on calf flexibility and strength can significantly reduce tightness. Chiropodists can recommend targeted stretches that target the gastrocnemius and soleus muscles — helping improve range of motion in the lower leg and fighting off stiffness.
Calf raises in particular (see demonstration below) can enhance muscle endurance and prevent recurring tightness. Incorporating these exercises into a daily routine can improve mobility and reduce the likelihood of calf-related discomfort.
Some other good examples of stretches for calf muscles include the Soleus Stretch and Heel Stands. Click the links for Feet First Clinic demonstrations!
https://www.youtube.com/shorts/ZVSfzY6so8w
March 13, 2025
Flat feet are a condition in and of themselves. However, flat feet also have an impact on future foot health and can lead to other more painful foot conditions. But can flat feet really cause bunions? While it seems unlikely that a toe deformity can be linked to a flat arch, you'd be surprised how interconnected our lower extremities are, especially the feet! Today’s article will explore how flat feet cause bunions, what you can do to prevent them, and how a foot specialist like a Chiropodist or Podiatrist can provide treatment.
What are Flat Feet?
Flat feet, or pes planus, cause the entire sole or most of it to contact the ground when standing and walking. For some people, this condition can extend into adulthood from childhood (children have flat feet before the arch forms) when the arch fails to form.When you have normal arches, they provide an elastic, springy connection between the forefoot and the hindfoot, allowing forces incurred during weight-bearing to be distributed properly. When these arches don’t exist, this mechanism is disrupted, leading to pain and other complications.
What are Bunions?
https://www.youtube.com/shorts/sXF8lWHad0g
Bunions, or hallux valgus, are bony protrusions that form on the inside edge of the first metatarsophalangeal (MTP) joint at the base of the big toe. They develop when pressure causes the big toe to deviate toward the second toe, resulting in a misalignment of the joint. Emerging research indicates that hypermobility in the midfoot (specifically the mid-tarsal joint between the navicular and the base of the first metatarsal) may be a key underlying factor in the development of bunions, and this hypermobility is often genetic.
Common Bunion Causes and Risk Factors:
Ill-Fitting Footwear: Wearing the wrong shoes for years is a major risk factor for most foot conditions, especially bunions. Wearing tight, narrow, or high-heeled shoes can exacerbate pressure on the big toe joint, contributing to bunion formation. Your toes need space to splay and rest comfortably!
Gender and Age: Women, particularly those over 60, are more prone to developing bunions, generally due to decades spent making poor footwear choices, or possibly due to hormonal influences that affect the ligaments in the foot.
Inflammatory Conditions: Diseases like rheumatoid arthritis can cause joint inflammation, which increases stress on the big toe and the risk of bunions.
Foot Injuries: Trauma to the foot can alter its mechanics, leading to bunion development.
https://www.youtube.com/shorts/KZiVzLyBUMo
Flat Feet and Bunions: The Connection
If you’re not proactive, the shape of your foot arch can have a big impact on our foot health over time. You may know that flat feet can lead to plantar fasciitis, and you may also know that high arches can lead to back pain, but our arch shape can affect us in countless ways. Let’s talk about the science behind why a flat foot can lead to a painful bunion.
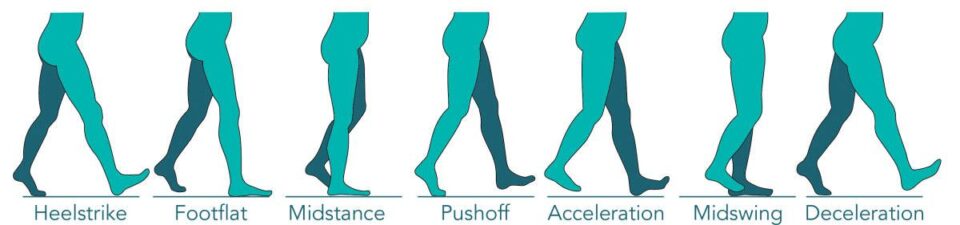
It all boils down to flat feet causing an abnormal gait (walking pattern), and the damage caused by walking with that abnormal pattern for a long period of time.The structural anomaly of flat feet and barely having an arch, or no arch at all, can significantly impact foot mechanics—particularly during walking. In a typical gait cycle, the foot pronates (rolls inward) to absorb shock and then supinates (rolls outward) to create a rigid lever for propulsion. Individuals with flat feet often experience overpronation, where the foot remains excessively rolled inward during the push-off phase. The altered biomechanics increases pressure on the first MTP joint, leading to instability and misalignment. Over time, this persistent stress can cause the big toe to deviate toward the second toe, resulting in a bunion.
Moreover, flat feet can lead to muscle imbalances that exacerbate bunion formation. Weakness in the intrinsic foot muscles (a group of tiny muscles inside the foot) and the tibialis posterior muscle (a muscle in your lower leg) compromises arch support, worsening overpronation. This chain reaction places additional strain on the big toe joint, accelerating bunion development. Therefore, the combination of altered foot mechanics and muscle imbalances associated with flat feet plays a significant role in the development and progression of bunions.
https://www.youtube.com/shorts/pdyv58z1D2Y
Preventing Bunions With Flat Feet
First and foremost, it’s all about the shoes! Selecting footwear that fits properly with a wide toe box and adequate arch support is crucial. A spacious toe box prevents crowding of the toes, reducing pressure on the big toe joint and minimizing the risk of bunion formation. Adequate arch support helps maintain proper foot alignment, distributing weight evenly and alleviating stress on MTP joint. Avoiding high heels and narrow shoes is essential, as they can exacerbate foot misalignment and increase the likelihood of developing bunions.
Incorporating custom orthotics can provide even more arch support if you have flat feet. These orthotics help correct overpronation—which we know now is a common issue—by stabilizing the foot's movement during the gait cycle and keeping it in neutral alignment. By improving foot alignment, orthotics reduce undue pressure on the big toe joint, reducing your risk of bunion development.
Lastly, Engaging in specific exercises can strengthen the muscles supporting the foot arch, enhancing stability and function. These exercises should aim to:
Strengthen Foot Muscles: Targeting the intrinsic and extrinsic muscles of the foot to provide better support for the arch and improve overall foot stability.
Improve Flexibility: Enhancing the range of motion in the toes, feet, and ankles to prevent stiffness and reduce strain on the MTP joint.
Enhance Balance and Coordination: Developing proprioception to ensure proper foot placement and gait mechanics, thereby reducing the risk of misalignment.
Regular practice of these exercises can improve foot biomechanics, reduce overpronation, and subsequently lower the risk of bunions. See below for an example of a great flat foot exercise.
https://www.youtube.com/shorts/whJ3TZAOn00
Foot Clinic Bunion Care
If you already struggle with bunions and foot pain, don’t worry; there are plenty of options available to you.
Bunions cannot be reversed after they form, but they can be managed with guided care from a podiatrist or chiropodist. The goal is to avoid invasive surgical intervention while still preventing bunions from impacting your daily life as much as possible. Most of these bunion treatment options are available at our downtown Toronto foot clinic:
Footwear Modification. Wearing shoes with a wide toe box and avoiding high heels can help reduce pressure on the bunion. Orthopedic shoes designed to accommodate bunions provide additional support and comfort.
Anti-inflammatory Medication. Over-the-counter NSAIDs, such as ibuprofen, can help reduce inflammation and alleviate pain associated with bunions.
Bunion Splints and Aligners. Devices like bunion splints and toe spacers can help realign the big toe and reduce discomfort. They can provide symptomatic relief, and you can try a more rigid device if your bunion is severe.
Therapeutic Taping. Applying tape to the foot can help maintain proper alignment and reduce strain on the bunion, providing temporary relief from pain and inflammation.
Shoe Stretching. Professional shoe stretching can create additional space in the shoe, reducing pressure on the bunion without altering the overall size of the footwear.
Supportive Insoles or Custom Orthotics. Custom orthotics can provide support to the arches and correct faulty biomechanics. This can potentially slow the progression of bunions by reducing pressure on the first MTP joint.
Bunion Exercises. Strengthening foot muscles through specific exercises can improve joint stability and decrease bunion-related pain. Try these 5 simple exercises for bunions.
Shockwave Therapy: This non-invasive treatment can address tight muscles and soft tissue injuries associated with bunions. This can potentially reduce pain and improve function.
Implementing these non-surgical interventions can significantly alleviate discomfort and slow the progression of bunions, enhancing overall foot health and quality of life.
https://www.youtube.com/shorts/8g43ZWreZ1g